BIGBEAR
PHARMACEUTICAL
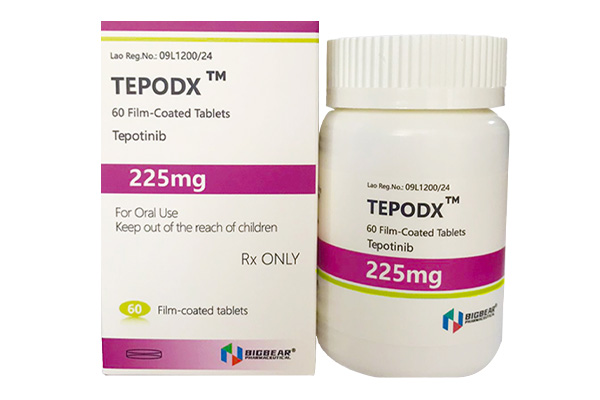
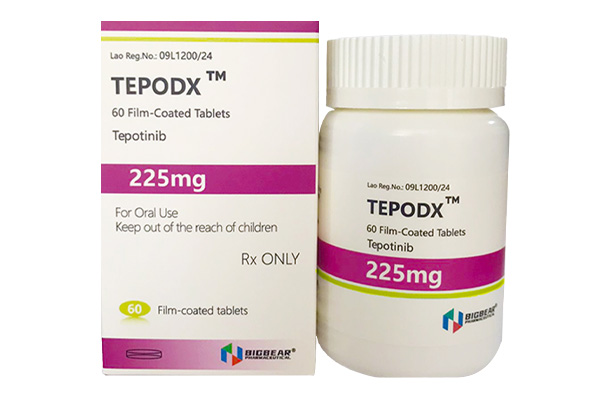
Tepotinib inhibits the phosphorylation of MET, blocks downstream signal transduction, and suppresses the proliferation.

 Authentic
Authentic Guarantee
Guarantee Fast Delivery
Fast Delivery Privacy
Privacy Tepotinib is an oral kinase inhibitor that primarily acts on the MET receptor tyrosine kinase. It is indicated for adult patients with metastatic non-small cell lung cancer (NSCLC) who have been confirmed to harbor MET exon 14 skipping mutations by detection.
This product is indicated for the treatment of adult patients with locally advanced or metastatic non-small cell lung cancer (NSCLC) who harbor a mesenchymal-epithelial transition factor (MET) exon 14 skipping mutation.
Prior to initiating treatment with this product, a fully validated detection method (liquid biopsy or tumor tissue biopsy) must be used to confirm the presence of a MET exon 14 skipping mutation.For patients from whom tumor tissue biopsy is not feasible, it is recommended to test plasma samples for the MET exon 14 skipping mutation. If no mutation is detected in plasma, the feasibility of obtaining a tumor tissue biopsy should be re-evaluated.
The recommended dose of tepotinib is 450 mg (2 tablets) once daily, taken with food, until disease progression or unacceptable toxicity occurs.
Instruct patients to take the tablets at approximately the same time each day, swallowed whole. Do not chew, crush, or split the tablets.
If a missed dose is remembered less than 8 hours before the next scheduled dose, the missed dose should not be taken.
If vomiting occurs after a dose, the patient should take the next dose at the scheduled time.
To manage adverse reactions, the recommended dose reduction is to 225 mg (1 tablet) once daily.Patients who cannot tolerate 225 mg once daily should permanently discontinue treatment.
Any grade: If ILD is suspected, temporarily discontinue the medication. If ILD is confirmed, permanently discontinue treatment.
Grade 3: Temporarily discontinue until ALT/AST levels return to baseline. If recovery occurs within 7 days, resume treatment at the same dose; otherwise, resume at a reduced dose.
Grade 4: Permanently discontinue treatment.
ALT/AST > 3x ULN and total bilirubin > 2x ULN: Permanently discontinue treatment.
Grade 3: Temporarily discontinue until bilirubin levels return to baseline. If recovery occurs within 7 days, resume treatment at a reduced dose; otherwise, permanently discontinue.
Grade 4: Permanently discontinue treatment.
Grade 2: Maintain the current dose if tolerated. If not tolerated, temporarily discontinue until recovery, then resume at a reduced dose.
Grade 3: Temporarily discontinue until recovery, then resume at a reduced dose.
Grade 4: Permanently discontinue treatment.
1.Females of reproductive potential are recommended to undergo a pregnancy test before initiating tepotinib treatment.
2.Females of reproductive potential should use effective contraception during treatment with tepotinib and for at least 1 week after the last dose.
3.Patients using systemic hormonal contraceptives should add a barrier method of contraception during treatment with tepotinib and for at least 1 week after the last dose.
4.Male patients with female partners of reproductive potential should use a barrier method of contraception during treatment with tepotinib and for at least 1 week after the last dose.
No human data on the effects of tepotinib on fertility are available.
In repeated-dose toxicity studies, no morphological changes were observed in male or female reproductive organs.
There are no clinical data on the use of tepotinib in pregnant women.
1.Animal studies have shown that this product is teratogenic (see [Pharmacology and Toxicology]). Based on the mechanism of action of tepotinib and animal study results, administration to pregnant women may cause fetal harm.
2.Tepotinib should not be used during pregnancy unless the clinical condition of the patient requires treatment with tepotinib and the potential benefit outweighs the risk.
3.Advise females of reproductive potential and male patients with female partners of reproductive potential of the potential risk to the fetus.
There are no data on whether tepotinib or its metabolites are excreted in human milk, or on their effects on breastfed infants or milk production.
Breastfeeding should be discontinued during treatment with tepotinib and for at least 1 week after the last dose.
Mild to moderate impairment (creatinine clearance 30–89 mL/min): No dose adjustment is required.
Severe impairment (creatinine clearance < 30 mL/min): The recommended dose has not been established.
Mild (Child-Pugh A) to moderate (Child-Pugh B) impairment: No dose adjustment is required.
Severe (Child-Pugh C) impairment: The recommended dose has not been established.
No dose adjustment is required for patients aged 65 years and older.
The safety and efficacy of tepotinib in children and adolescents under 18 years of age have not been established.
At the recommended dose for the target indication, the most common adverse reactions occurring in ≥20% of tepotinib-exposed patients (N=313) are as follows:
The most frequent adverse reaction was edema (81.5% of patients), primarily peripheral edema (72.5%).
Other common adverse reactions included hypoalbuminemia (32.9%), nausea (31.0%), increased creatinine (29.1%), and diarrhea (28.8%).
The most common serious adverse reactions were:
Peripheral edema (3.2%)
Generalized edema (1.9%)
Interstitial lung disease (ILD) (1.0%)
24.9% of patients permanently discontinued treatment due to adverse reactions.
The most common adverse reactions leading to permanent discontinuation (≥1% of patients) were:
Peripheral edema (5.4%)
Edema (1.3%)
Genital edema (1.0%)
ILD (1.0%)
52.7% of patients temporarily interrupted treatment due to adverse reactions.
The most common adverse reactions leading to temporary interruption (≥2% of patients) were:
Peripheral edema (19.8%)
Increased creatinine (5.8%)
Generalized edema (4.8%)
Edema (3.8%)
Increased alanine aminotransferase (ALT) (2.9%)
Nausea (3.2%)
Increased amylase (1.6%)
36.1% of patients required dose reduction due to adverse reactions.
The most common adverse reactions leading to dose reduction (≥2% of patients) were:
Peripheral edema (15.7%)
Increased creatinine (3.2%)
Edema (2.6%)
This product is contraindicated in patients with a known hypersensitivity to the active ingredient or any of the excipients.
Interstitial lung disease (ILD) or ILD-like adverse reactions, including pneumonitis, have been reported in patients receiving monotherapy with tepotinib at the recommended dose, and may be fatal.
Monitor patients for pulmonary symptoms suggestive of ILD. If such symptoms occur, immediately suspend tepotinib and promptly evaluate the patient for a definitive diagnosis of ILD or other specific causes. If ILD is confirmed, permanently discontinue tepotinib and provide appropriate treatment.
Elevations in alanine aminotransferase (ALT) and/or aspartate aminotransferase (AST), including a fatal case of hepatic failure, have been reported in patients receiving monotherapy with tepotinib at the recommended dose.
Monitor liver enzymes (ALT, AST) and bilirubin prior to initiating tepotinib, and thereafter as clinically indicated. If Grade 3 or higher elevations occur (ALT and/or AST > 5x ULN), dose adjustment or treatment interruption is recommended.
Cases of QTc interval prolongation have been reported, but the number of patients affected is limited.
For patients at risk of QTc prolongation, including those with known electrolyte abnormalities or those receiving concomitant medications that prolong the QTc interval, monitoring is recommended when clinically indicated (e.g., ECG, electrolytes).
Administration of tepotinib to pregnant women may cause fetal harm.
Pregnancy testing is recommended for females of reproductive potential prior to initiating treatment. Advise females of reproductive potential and male patients with female partners of reproductive potential of the potential risk to the fetus.
Females of reproductive potential and male patients with female partners of reproductive potential should use effective contraception during treatment with tepotinib and for at least 1 week after the last dose.
Concomitant use with strong CYP and P-gp inducers or dual strong CYP3A and P-gp inhibitors should be avoided.
In vitro studies have shown that tepotinib or its major metabolites can inhibit renal tubular transporters, including organic cation transporter (OCT) 2 and multidrug and toxin extrusion (MATE) transporters 1 and 2. Creatinine is a substrate of these transporters.
Elevations in serum creatinine may result from inhibited active tubular secretion, rather than renal injury. Due to this effect, renal function estimates relying on serum creatinine (e.g., creatinine clearance, estimated glomerular filtration rate) should be interpreted with caution. If serum creatinine increases during treatment, further evaluation of renal function is recommended to rule out renal impairment.
This product contains lactose. Patients with rare hereditary disorders of galactose intolerance, total lactase deficiency, or glucose-galactose malabsorption should not use this product.
If any issues arise, please contact us immediately.
Email:laosbigbear@gmail.com

Tepotinib is used in adults to treat non-small cell lung cancer that has spread to other parts of the body (metastatic).
Your doctor will make sure you have the correct tumor type to be treated with tepotinib. Tepotinib may also be used for purposes not listed in this medication guide.
Take the medicine as soon as you can, but skip the missed dose if your next dose is due within 8 hours. Do not take two doses at one time.
Other drugs may affect tepotinib, including prescription and over-the-counter medicines, vitamins, and herbal products. Tell your doctor about all other medicines you use.
Follow your doctor's instructions about any restrictions on food, beverages, or activity.
Copyright2024@ BIGBEAR All right reserved Bigbear | Bigbear Pharmaceutical | Bigbear Laos



